
https://www.gosh.nhs.uk/conditions-and-treatments/clinical-outcomes/dietetics-clinical-outcomes/
Dietetics clinical outcomes
Clinical outcomes are measurable changes in health, function or quality of life that result from our care. Constant review of our clinical outcomes establishes standards against which to continuously improve all aspects of our practice.
About the Dietetics service
The Dietetics Service at Great Ormond Street Hospital (GOSH) provides specialist nutrition assessment, intervention and ongoing management for infant, children’s and young people with acute and chronic health conditions across all the hospital’s specialist clinical services. Working as an integral part of the multidisciplinary team, we work to empower patients and families on how to manage their child’s nutrition during their hospital stay and when at home we support growth, optimise nutrition status and manage disease-related nutritional complications.
Clinical outcome measures
Blood, Cells and Cancer Dietetics team
The Blood, Cells and Cancer Dietetics Team works in close partnership with the clinical specialties of Haematology and Oncology, Bone Marrow Transplant, Immunology, Dermatology, Rheumatology, and Infectious Diseases. Children and young people with conditions treated by these specialties have a higher risk of malnutrition (e.g. caused as an effect of the disease itself or side effects of the treatment) and may have complex nutritional needs. The team assess the nutritional and dietary needs of patients and work to support nutrition, growth and long-term health.
Nutrition and Dietetic Patient Outcomes Questionnaires (NDPOQ)
Our Service captures outcomes from the perspective of parents and carers, and young people themselves (aged 8 and over) through the Nutrition and Dietetic Patient Outcomes Questionnaire (NDPOQ). The NDPOQ is a validated self-reported questionnaire developed for use with patients and their carers to inform the quality of the nutrition and dietetic care they receive. The NDPOQ gives us information about how our Dietetic Service assists with health-related knowledge and empowerment, and the effects of our care on daily living.
2023/24 Results
The results below are from parents and carers with a child receiving specialist nutrition and dietetic care from the Blood, Cells and Cancer Dietetics Team during August 2023 and June 2024 (54 responses). Due to a low number of responses from our children and young people, we are currently collecting further data with the aim to publish their results in 2026/27.
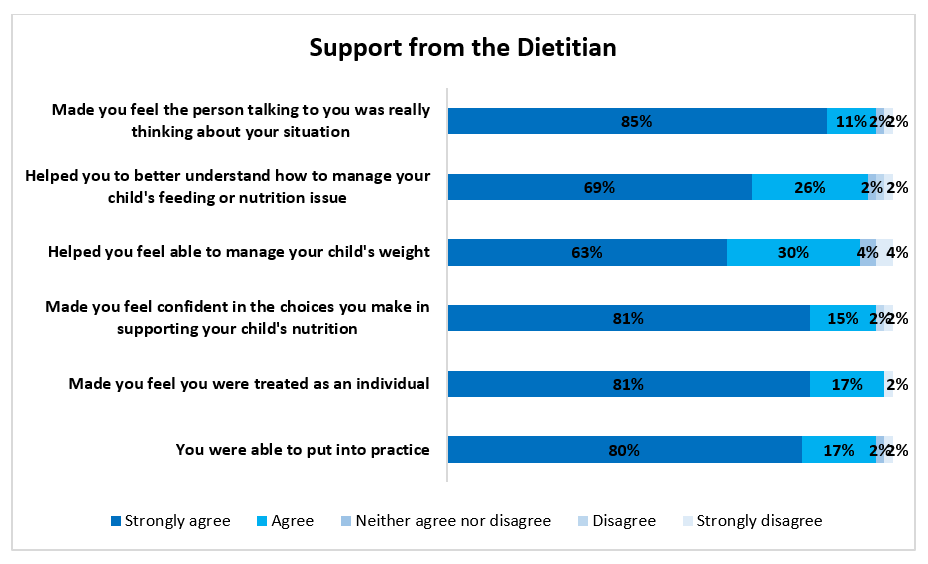
Figure 1. Blood, Cells and Cancer Dietetics service NDPOQ results: 2023/24
Satisfaction with the Dietetic service
When asked about their overall level of satisfaction with advice and support from the Dietetic service at GOSH, below were the responses from the parents/carers.
Thoughtful and personalized advice. Sensitive to both the nutritional and behavioural needs of the patient, alongside familial culture
Have always felt like my son was being treated as an individual and his needs were being met and responded to well and swiftly
I felt like I wasn’t judged, and I was made to feel like I was doing a good enough job
Best dietician we have ever met. Practical and informed advice. 10/10
…so reassuring whilst answering all my questions
They have always listened to my own anxieties about my child's weight loss and loss of appetite, they have been reassuring and always offered lots of good advice about calorie boosting his snacks and meals
…made me feel a million times better about our struggles with food and I felt much more positive about our situation afterwards
Continuous improvement
The 2023/24 NDPOQ feedback highlights the positive impact of the Blood, Cells and Cancer Dietetics Service, with parents and carers consistently emphasising personalised, responsive and compassionate care. Improvements were observed in patient satisfaction scores compared with previous years, likely reflecting the benefits of an increasingly established service. Although the results are encouraging, we have planned more targeted engagement methods for future data collection to increase the response rate from our children and young people. Ongoing service review will continue to prioritise preferred outpatient formats - particularly face‑to‑face and telephone consultations - while strengthening data collection to ensure that future quality improvements are shaped by the voices and experiences of those who use our service.