
https://www.gosh.nhs.uk/conditions-and-treatments/clinical-outcomes/anaesthesia-clinical-outcomes/
Anaesthesia clinical outcomes
Clinical outcomes are measurable changes in health, function or quality of life that result from our care. Constant review of our clinical outcomes establishes standards against which to continuously improve all aspects of our practice.
About the Anaesthesia Service
The department of Anaesthesia at Great Ormond Street Hospital (GOSH) is one of the UK's leading centres for the provision of anaesthesia and pain management for children requiring a wide range of surgical, radiological and medical procedures. In the last 12 months we have carried out 16,245 anaesthetics.
The department consists of 52 consultants and 30 specialist trainees that provide 24-hour dedicated paediatric anaesthesia services. We also have a leading role in education and training of doctors and other health professionals.
Clinical outcome measures
Our electronic patient record system (Epic) allows us to report outcomes on the entire patient population in real time. We currently measure and report on three specific anaesthetic clinical outcomes, although we are working on expanding this list to include others:
- Temperature on arrival to Post-Anaesthesia Care Unit (PACU)
- Pain scores on waking in PACU
- Incidence of post-operative nausea and vomiting (PONV) in PACU
All of the measures show natural variation over time, but are within expected range and show consistently good anaesthetic clinical outcomes for patients. We continue, through our ongoing quality improvement and audit programmes, to improve patient care and outcomes for children receiving anaesthesia and pain management at GOSH.
1. Temperature on arrival to Post-Anaesthesia Care Unit (PACU)
During anaesthesia and surgery, a child’s temperature can drop to below 36.0°C (hypothermia). Hypothermia is associated with a higher risk of complications after surgery. A range of warming devices are used during anaesthesia to prevent hypothermia.
A child’s temperature is measured at regular intervals before and during anaesthesia and on arrival to PACU.
The National Institute for Clinical Excellence (NICE) recommends that a patient’s temperature should be kept above or equal to 36.0°C in adults having surgery under anaesthesia. Although there are no current recommendations for children it is widely agreed that avoidance of hypothermia in children undergoing surgery (excluding heart surgery) is beneficial.
Figure 1: Percentage of patients arriving in PACU with a temperature less than 36.0°C
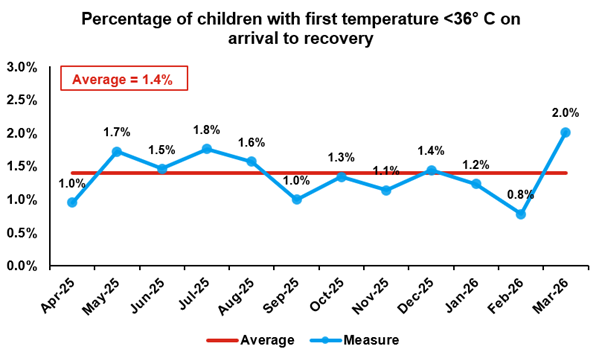
This graph shows that, on average, 1.4% of our patients are arriving in recovery with a temperature less than 36°C.
2. Pain scores on wakening
Pain-relieving drugs are given by the anaesthetist during surgery to ensure that children are as comfortable as possible after surgery. The type and strength of pain relief given will depend on the procedure. After surgery, the specialist nurse in the PACU will assess if the child is comfortable using a simple zero to 10 scale (no pain at zero and worst possible pain at 10). If necessary, the child will receive further pain relief to ensure they are comfortable before going to the ward.
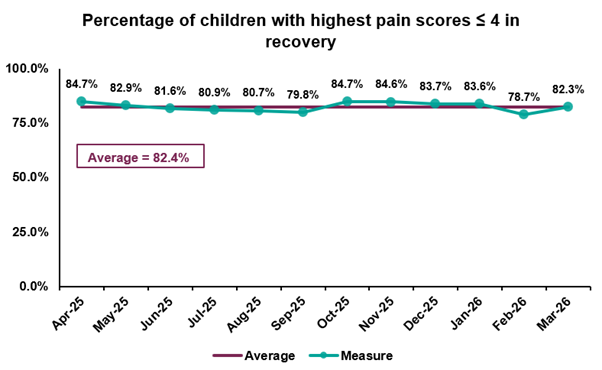
The graph below shows that, over the past 12 months, an average of 82.4% of patients in Recovery had a highest pain score of 4 or less (suggesting zero or mild pain). This is in line with our historical average. We apply the same target as Cincinnati Children’s Hospital – to seek to achieve more than 90% of children arriving comfortable in recovery. However, despite a good result, we also share a commitment to continuous improvement, so we expect to increase this score over time.
Figure 2: Percentage of patients wakening in PACU with a pain score of four or less
3. Incidence of post-operative nausea and vomiting (PONV)
Some children may suffer sickness (vomiting) or nausea (feeling sick) after anaesthetics. The degree of risk will depend on the child’s medical condition and the nature of surgery for which anaesthesia is being provided. It can usually be prevented or treated effectively.
Figure 3: Percentage of patients that experience nausea or vomiting in PACU
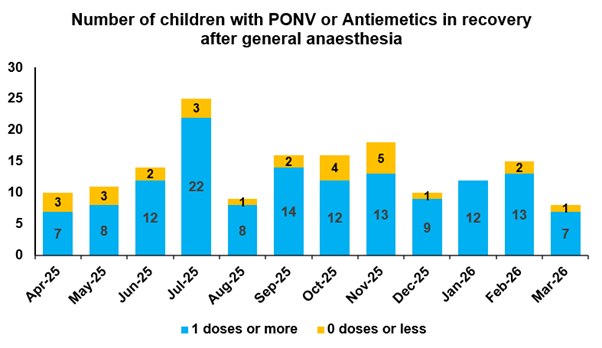
The graph above shows that on average, fewer than 20 children per month require additional antiemetics or suffer from PONV in recovery. This is less than 1% of the total patient cohort and is an improvement on our historical averages.
Continuous improvement
The department of anaesthesia uses this data along with other measures to ensure we maintain delivery of high quality and expert care. It also allows us to identify opportunities for improvement.