
https://www.gosh.nhs.uk/conditions-and-treatments/clinical-outcomes/plastic-surgery-clinical-outcomes/
Plastic Surgery Clinical Outcomes
Clinical outcomes are measurable changes in health, function or quality of life that result from our care. Constant review of our clinical outcomes establishes standards against which to continuously improve all aspects of our practice.
About the Plastic and Reconstructive Surgery Service
We see children with a wide range of conditions both present at birth (congenital) or developed in childhood. Children who need plastic or reconstructive surgery are seen as outpatients, day care patients or inpatients.
As well as our thirteen consultant plastic surgeons, the surgical team consists of specialist registrars, fellows in hand, cleft and craniofacial surgery, and Trust doctors. Clinical nurse specialists, occupational therapists, physiotherapists and our departmental administrative team complete the Plastic and Reconstructive Surgery Department.
Our special areas of expertise include:
- craniofacial surgery
- cleft lip and palate repair
- congenital hand anomalies
- ear surgery
- facial palsy
- vascular anomalies and birthmarks
- general plastic and reconstructive surgery.
Clinical outcome measures
1. Non-elective re-admission rate within 30 days to any specialty after a procedure under the plastic surgery specialty
Complications resulting from surgery can occasionally cause patients to be readmitted to hospital. The rate of readmissions is a standard hospital outcome that is monitored to reduce complications and improve care. The table below shows the number of patients discharged from the Plastic Surgery specialty who have a non-elective (emergency) readmission within 30 days of discharge (excludes day cases).
Numerator: number of inpatient discharges under the Plastic Surgery specialty that have a subsequent non-elective readmission within 30 days of discharge from GOSH.
Denominator: number of all inpatient discharges from GOSH under the Plastic Surgery specialty. Day cases are excluded.
Table 1 Non-elective re-admission rate within 30 days to any specialty after a procedure under the Plastic Surgery specialty
| Year |
Patients requiring non-elective readmission within 30 days |
Total number of all inpatients discharged under plastic surgery specialty |
Percentage of readmissions within 30 days |
|---|---|---|---|
| 2021/22 | 3 | 298 | 1.01% |
| 2022/23 | 9 | 340 | 2.65% |
| 2023/24 | 3 | 307 | 0.98% |
| 2024/25 | 3 | 336 | 0.89% |
| Total | 18 | 1,281 | 1.41% |
2. Unscheduled return to theatre within seven days under any specialty after a procedure under the plastic surgery specialty
Due to the complexity of some operations or related to complications during surgery, a small number of patients may need further surgery that was unplanned. To help reduce this occurrence and its potential effects on outcome and patient experience, we monitor the rate of patients who return to theatre soon after a procedure. The table below shows the number of patients who have an unscheduled return to theatre within seven days of previous scheduled surgery under the Plastic Surgery specialty.
Numerator: number of unscheduled theatres cases (any specialty) within seven days of previous scheduled theatre case under the Plastic Surgery specialty.
Denominator: number of scheduled theatres cases under the Plastic Surgery specialty.
Table 2 Unscheduled return to theatre within seven days under any specialty after a procedure under the Plastic Surgery specialty.
| Year |
Patients returning unscheduled to theatre within 7 days |
Total number of scheduled theatre cases under the plastic surgery specialty. |
Percentage of patients returning unscheduled to theatre within 7 days |
|---|---|---|---|
| 2021/22 | 8 | 795 | 1.01% |
| 2022/23 | 7 | 796 | 0.88% |
| 2023/24 | 5 | 770 | 0.65% |
| 2024/25 | 7 | 854 | 0.82% |
| Total | 27 | 3,215 | 0.84% |
International clinical outcome measure development
Our team of plastic surgeons are advocates for and have helped to develop validated outcome measures and define minimum data sets. We continue to develop the breadth of our data collection to demonstrate our outcomes.
- ICHOM | Craniofacial Microsomia Standard Set | Measuring Outcomes
- ICHOM | Paediatric Facial Palsy Standard Set | Measuring Outcomes
- ICHOM | Cleft Lip & Palate Standard Set | Measuring Outcomes
- ICHOM | Congenital Upper Limb Anomalies Standard Set
- EAR-Q | Q-Portfolio - MEASURING WHAT MATTERS TO PATIENTS
- FACE-Q | Craniofacial - Q-Portfolio MEASURING WHAT MATTERS TO PATIENTS
Occupational Therapy clinical outcome measures
Functional and cosmetic outcome measure following pollicisation surgery
The Congenital Hand Anomalies Service at GOSH is one of the largest in the UK, offering reconstructive hand surgery and therapy to children with a variety of conditions.
Thumb hypoplasia is a congenital condition where the child is born with a small or absent thumb. It is often associated with radial ray dysplasia (RRD), also known as radial club hand. This condition affects the development of the whole arm and is classified from mild (Type I) to severe (Type IV). Thumb hypoplasia can also be isolated, with no other anomalies affecting the upper limb. Thumb hypoplasia is frequently treated by pollicisation surgery. This complex surgery constructs a new thumb using the index finger. Following surgery, hand therapy is provided by the occupational therapists to help children maximize the movement, strength, function and appearance of their new thumb.
To gain a fuller understanding of pollicisation surgery, please view the film 'Making a thumb' from the Scottish Rite Hospital in Texas.
1. Patient-Reported Outcome Measure of thumb function and appearance
The Patient-Reported Outcome Measure (PROM) was developed by the Occupational Therapists to provide an insight into the parent and patient’s perspective of surgical outcome. It asks about type and frequency of thumb use, movement, strength, function and appearance. Parents or carers completed the PROM for children under 6 years of age. Children and young people aged 6 to 18 completed it themselves. The PROM results below include all types of thumb hypoplasia, including isolated and those associated with RRD.
We gathered data over a two-year period 2023-2024 and saw 32 patients who had pollicisation. For those patients that attended in both years, we considered only the latest assessments. This left us with 26 patients. Of those, four patients had both hands operated, so in total, we considered 30 hand assessments for this review.
| 1. Do you use your thumb? | |
|---|---|
|
I use my thumb spontaneously in daily tasks (27/30) |
90% |
|
I use my thumb in daily tasks only when prompted / reminded (3/30) |
10% |
| I never use my thumb (0/30) | 0% |
|
2. How often do you use your thumb to pick up large objects (eg a bottle)? |
|
|---|---|
| Often (17/30) | 57% |
| Sometimes (13/30) | 43% |
| Never (0/30) | 0% |
|
3. How often do you use your thumb to pick up small objects (eg a pea)? |
|
|---|---|
| Often (14/30) | 47% |
| Sometimes (14/30) | 47% |
| Never (2/30) | 6% |
|
4. How often do you use your thumb to manipulate small objects (eg doing up a button)? |
|
|---|---|
| Often (13/30) | 43% |
| Sometimes (11/30) | 37% |
| Never (6/30) | 20% |
The majority of patients (90%) report to use their thumb spontaneously in daily tasks, 10% when prompted or reminded and 0% reported never to use their thumb.
We asked how frequently patients use their thumb to pick up large objects and 57% reported to do this often, 43% reported sometimes and 0% reported never.
We asked how frequently patients use their thumb to pick up small objects and 47% reported often, 47% reported sometimes and 6% reported never.
When we asked how frequently patients use their thumb to manipulate small objects and 43% reported often, 37% reported sometimes and 20% reported never.
|
Following your surgery, how satisfied are you with… |
Dissatisfied |
Neither satisfied nor dissatisfied |
Satisfied |
|---|---|---|---|
|
The appearance of your thumb (how it looks)? |
3/30 (10%) | 7/30 (23%) | 20/30 (67%) |
| The movement of your thumb? | 3/30 (10%) | 13/30 (43%) | 14/30 (47%) |
|
The function of your thumb (how it works)? |
1/30 (3%) | 11/30 (37%) | 18/30 (60%) |
| The strength of your thumb? | 7/30 (23%) | 12/30 (40%) | 11/30 (37%) |
The majority of patients report to be satisfied with the appearance of their thumb (67%), their movement (47%) and function (60%). Thumb strength was reported to have the lowest level of satisfaction (37%).
2. Occupational Therapist assessment of strength
In addition to the PROM, the 6-to-18-year-olds were also assessed for grip and pinch strength.
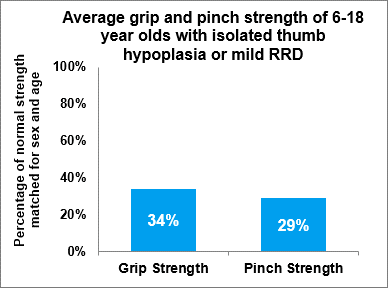
Fig 2.1 Average grip and pinch strength in 6-18 year-olds with isolated hypoplasia or very mild (type 1) RRD (N=14), 2023-2024
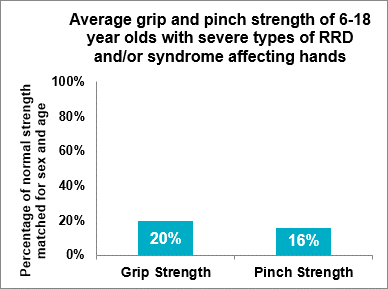
Fig 2.2 Average grip and pinch strength of 6-18 year-olds, with types 2 to 4 RRD (N=8), 2023-2024
The results displayed are compared with normal population data, matched for sex and age. They demonstrate that following pollicisation surgery, grasp and pinch strength is always significantly less than normal, and the more severe the associated condition of RRD, the weaker the grip and pinch. For people with isolated thumb hypoplasia and mild RRD (type 1), average grip strength post-operatively is 34% of normal, and pinch strength is 29% of normal. For people with more severe RRD, average grip strength post-operatively is 20% of normal, and pinch strength is 16% of normal.
Conclusion
The results of our PROM suggest pollicisation surgery is an effective treatment to improve the movement, function and appearance of the hand in children and young people with thumb hypoplasia. The pollicised digit is always significantly weaker when compared to normal thumb strength and has the lowest level of satisfaction. Patients report to using their thumb to pick up large objects more frequently than to pick up and manipulate small objects. Overall, the patients and families who have undergone pollicisation are satisfied with the outcome of their surgery.
Continuous improvement
We aim to direct all patients considering pollicisation surgery to this website to learn about our outcomes. This data helps our families to make informed decisions about surgery.
References
McQuiddy, V. A. et al. Normative Values for Grip and Pinch Strength for 6- to 19-Year-Olds, Archives of Physical Medicine and Rehabilitation, 96:1627-33 (2015)
Netscher, D. T. et al. Functional Outcomes of Children With Index Pollicizations for Thumb Deficiency, The Journal of Hand Surgery, 38:250-257 (2013)
de Kraker M. et al. Outcome after pollicization: comparison of patients with mild and severe longitudinal radial deficiency, Plastic and Reconstructive Surgery, 131:544e-551e (2013)